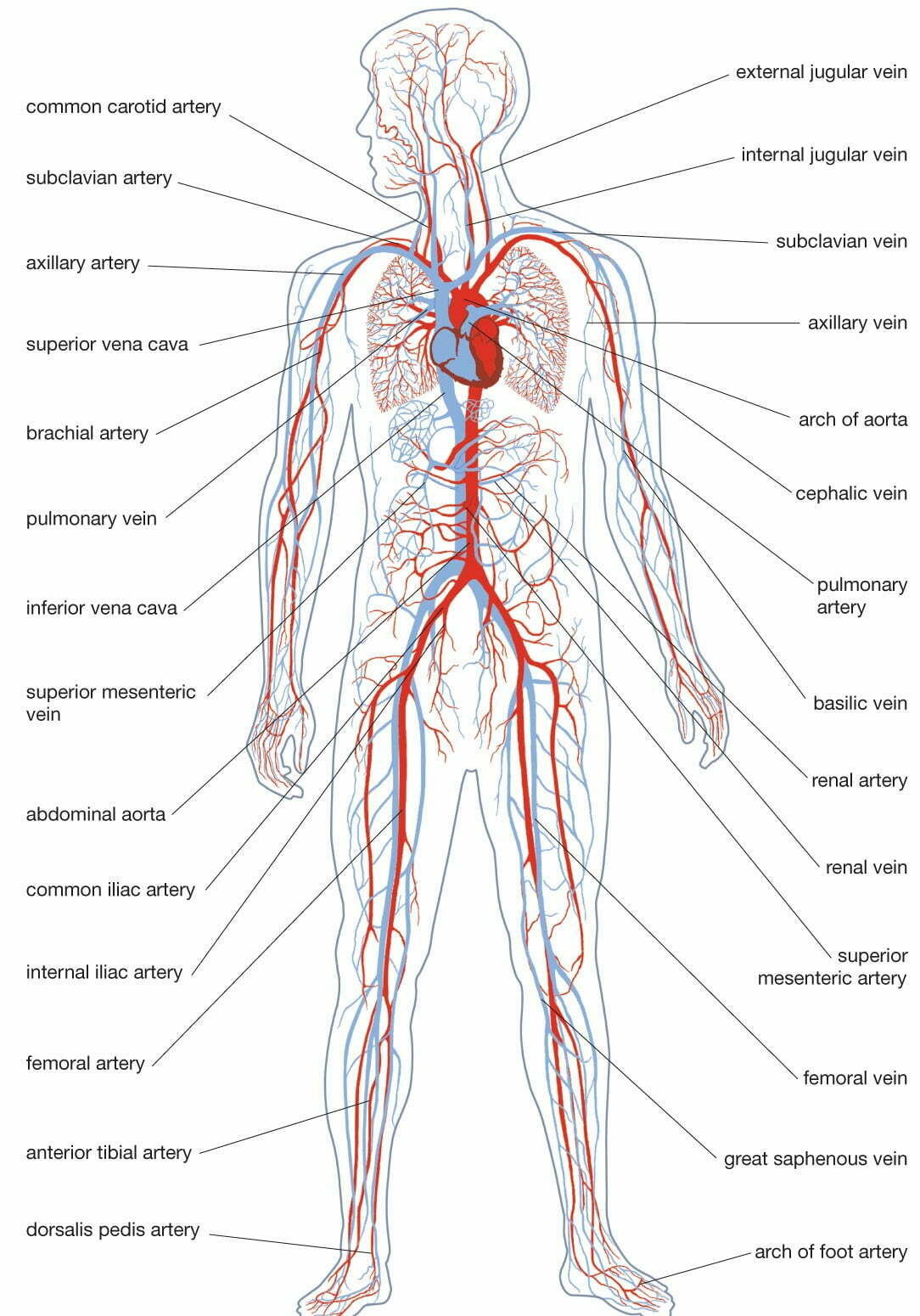
A four-week-old human embryo already has miles of blood vessels. By adulthood, we each have 60,000 miles of blood vessels inside our bodies – that’s more than twice the distance around the world.
Those vessels keep blood flowing, supplying your tissues with oxygen and nutrients and keeping your organs, including the heart, healthy.
In the embryo, specialised cells form the blood vessel lining, while other cells build up into the layers of the blood vessel.
The vessels are constructed all around the body, then join together to make the whole circulatory system. This activity is much slower in adulthood, but we never lose the ability to grow new blood vessels.
It is a process that helps the body heal when we get an injury but also has the potential to treat many conditions where something goes wrong with the blood vessels – including heart failure after a heart attack, diabetes, peripheral arterial disease and some types of stroke.
When part of your body needs new blood supply, something starts to happen in a nearby blood vessel. The endothelial cells – which form the lining of the blood vessel – start to multiply. Then they become shape-shifters.
Instead of flat cells, tightly bound together like bricks in a tunnel wall, they form a line, which heads off to where it is needed. Once the line reaches its destination, the cells rearrange back into tunnels.
This becomes the blood vessel and the cells remake the tight bonds that stop any blood leaking out.
Scientists already know Vascular Endothelial Growth Factor (VEGF) plays an important role. Scientists have tried injecting VEGF into tissues that have been damaged, to try to encourage new blood vessels to grow. But it turns out it’s more complicated than this, explains Professor Mellor.
“You get new blood vessels if you do this but they are not very good blood vessels – they don’t really last. If we have a more sophisticated understanding of the processes, then we can find drugs to target those processes, so we have been focusing on trying to understand the shape changes and movement of the cells.”
Professor Mellor and his team are experts in the cytoskeleton – the framework of every cell. Like our own skeleton, it controls the shape of the cell and its ability to move, but it’s more flexible than a human skeleton, able to expand, shrink or change shape as needed.
The team has discovered the role played by two proteins that allow cells to change shape. They’ve teamed up with international collaborators to study one of these in more detail: a protein with the snappy name of FMNL3.
How could research into blood vessels help those with heart and circulatory conditions?
“FMNL3 is part of a family of proteins that you find in nearly every living organism from yeast upwards – all plants and everything in the animal kingdom has them,” says Professor Mellor.
“These proteins seem to have a general function to allow cells to stretch and elongate. When plants produce long shoots, those are made by these proteins. When human nerve cells (which are incredibly long cells) stretch out, this occurs through these proteins. Now we know that this family of proteins are involved in blood vessels, too.”
If new blood vessels could be produced quickly, before the heart muscle dies, this research could even help repair hearts, that have been damaged by a heart attack.
To the researchers’ surprise, there is a form of this protein that controls blood vessels specifically. “It seems that evolution has designed some proteins that are specialised to help blood vessels change shape,” says Professor Mellor.
“This is good news because it’s easier to develop a drug to help this process if there is a specific protein that you can target, which isn’t also involved in all the other kinds of cells in your body.”
In future, they hope to work with other scientists on a drug that could improve this process, which could help people with damage to blood vessels, especially those with diabetes.
And there’s a bigger challenge for the future – if new blood vessels could be produced quickly before the heart muscle dies, this research could even help repair hearts that have been damaged by a heart attack.